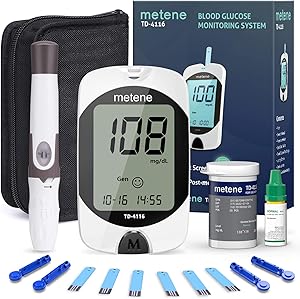
Diabetes Testing Kit, 50 Glucometer Strips, 50 Lancets, 1 Blood Glucose Monitor, metene TD-4116 Blood Sugar Test Kit with Lancing Device and Control Solution, No Coding
- Excellent Accuracy: metene TD-4116 blood glucose meter and strips are produced with industry-leading chips and biosensor, equipped with industry-leading technologies, conducive to get accurate and reliable measurements
- No Coding: The blood sugar meter gets into measure status automatically once insert the blood sugar test strip to the bottom of the slot, easy to use and easy to read with large display for the senior
- Fast and Reduce Pain: This blood glucose monitor takes just 7s and 0.7µl blood to get the glucose value; The lancing device has 5 depth options to minimize wound and reduce pain
- Better Data Management: This glucometer stores the newest 450 blood glucose values and display the continuous 14/21/28/60/90 day average; the measurements could be exported with windows-based software; help you track and manage your blood glucose better
- Diabetes Testing Kit 107 Piece Set: 50 glucometer strips, 50 30G lancets, 1 blood sugar meter, 1 lancing device, 1 control solution, 2 batteries, 1 protective wallet and 1 user manual; Please feel free to contact us if any problem when using this Diabetes testing kit
Blood glucose test
Blood glucose test 1
Blood glucose testing, also known as blood glucose self-monitoring (AMGS), is a method used to check how much glucose (sugar) is in the blood using a glucose meter, and can be done at any time and place. Your doctor can also check your glucose from a laboratory sample of blood.
- Target ranges for adults (except pregnant women) *
- Before meals 80-130 mg / dl (4.4-7.2 mmol / l)
- After meals Less than 180 mg / dl (10.0 mmol / l)
Your doctor uses the HbA1c (glycosylated hemoglobin) test to find out what your average blood glucose level has been over the past three months. This test, suitable for all types of diabetes, gives you and your doctor an indication of how well you are responding to the treatment plan. The recommended goal is to keep the level below seven percent (7%). Your doctor will tell you what the right goal is for you. The HbA1c test is sometimes called a hemoglobin A1c or glycated hemoglobin test.
The importance of self-analysis
Your HbA1c test result will not show the daily effects of your food choices and physical activity on your blood glucose levels. A glucose meter is a good way to learn about and monitor the immediate effects of food, physical activity, and other changes on your blood glucose levels, allowing you to take immediate action to bring your blood glucose levels down. place within the range recommended by your doctor. Your doctor may also use the results of your blood glucose meter, in addition to your HbA1c test result, to assess and adjust your treatment plan.
When to test * and what to consider: a practical guide
Use this simple chart as a guide on when to test and what to watch out for to help control your blood glucose levels on a daily basis, especially if you are taking insulin for diabetes.
When to test What to keep in mind
First thing in the morning, before eating or drinking How your body / medication controls blood glucose at night
Before meals
How effective is the dose of diabetes medicine between meals
Adjusting Your Food Choices (Carbohydrates) and Servings for Meal
Between one and two hours after meals The effect of food or medicine on your blood glucose levels
Before physical activity
Whether you should delay or postpone exercising
If you have a snack before you start exercising
During and after physical activity
How Physical Activity Affects Blood Glucose
Whether activity has delayed effects on blood glucose
Before bedtime If you need a snack before bed
Before driving If you need to delay driving and take steps to drive safely
According to the suggestions of the healthcare professional How well your treatment plan works
You may need to test your blood glucose more often * if:
- suffer from hypoglycaemia (low blood glucose) or hyperglycaemia (high blood glucose)
- start taking new diabetes medications that have been prescribed for you
- your dose of diabetes medicine has been adjusted
- try new foods
- is unwell or unwell
* Always check with your doctor when and how often you need to test your blood glucose.
How to Record Your Blood Glucose Results
You can always have a logbook close at hand in which to manually record your blood glucose measurements.
You'll find logbooks at your doctor's office, at healthcare centers, and even on the Internet. (Download one here )
Always update your blood glucose records and bring them to doctor visits. They can be used by healthcare professionals to determine the right treatment plan for you.
How to Monitor Your Blood Sugar Level
If you have diabetes , it is important to control your blood sugarbloodat different times of the day and throughout the year. There are 3 tools that can help you do this and therefore control your diabetes: A blood test that is done every three months, blood tests that are done every day, and a system that constantly monitors yourglucose in blood.
The 3-month blood test is called an A1C test. This test reflects your blood sugar (or blood glucose) control for the past 2 to 3 months. The best way for you and yourdoctorunderstand how well controlled your blood sugar levels are by testing your A1C level every 3 months. Your doctor will likely be the one who will order an A1C test. However, you can also purchase over-the-counter A1C test kits that you can use at home. Your A1C goal will be determined by your doctor. However, the goal is generally less than 7% or 8%, depending on your age.
The daily blood test is done with a blood glucose monitor (BGM). This is also called a blood sugar meter, glucometer, or glucose meter. It is often called self-monitoring of blood glucose. Your doctor may prescribe a BGM, especially if your blood sugar fluctuates. They will show you how to use it.
A BGM measures the amount of glucose in a dropof blood at that particular moment. This tried and true test is done by taking a sample of your blood, usually from your finger. This process is calledpuncturedigital. The blood from your finger is placed on a test strip and read on the monitor. Fingertips need to be done several times a day and sometimes at night to get avisionAccurate your glucose levels. Using a blood glucose monitor for regular tests throughout the day can help you improve control of your blood sugar levels. The results you get from your fingerstick show if your blood glucose is within the range set by your doctor. You can use these results to make appropriate adjustments to your diet , activity ,insulinor the doses of other medications. In many cases, the BGM results can be uploaded to a computer for reporting.
The third type of monitoring is with a continuous glucose monitoring system (CGM). This new product allows people with diabetes to measure their blood glucose throughout the day. CGMs involve a small, easy-to-insert sensor that is worn for 14 days. The sensor has an adhesive that helps it adhere to your skin. The CGM also includes a transmitter. This can be a separate device or it can be built into the sensor. Some CGMs last longer than 14 days, but must be placed under your skin by your doctor.
A CGM also comes with a receiver or reader. This allows your computer or smartphone to receive the data from the transmitter. The data provides detailed information and trends about your blood glucose throughout the day. Based on that, you can predict dangerous ups and downs before they happen. This can help you make quick daily adjustments to stay in your target area. Some adjustments include changes in your eating habits and level of exercise . Also, this information can help you and your doctor make decisions about managing your diabetes. If you wish, the data can be shared with someone you trust.
The path to better health
What supplies do I need?
You will need a glucose meter, alcohol swabs, finger lancets sterilees (small needles) and sterile test strips. A CGM comes as a complete kit, which includes a sensor, a transmitter, and a receiver or reader.
How do I select a glucose meter?
Your doctor will make a recommendation. Check with your health insurance plan to find out if they will pay for your glucose meter. If so, your plan may only pay for a certain meter.
Compare prices and costs. Consider what features are important to you. For example, some meters are made for people with low vision. If you want to pay a little more money, you can get a meter that stores the results in its memory. This allows you to compare results from several days at a time.
How do I measure my blood sugar level?
Follow your doctor's advice and the instructions that come with your glucose meter. Different meters work differently, so be sure to check with your doctor for advice specific to you. With a BGM, you will normally follow the steps below:
- Wash your hands and dry them well before testing.
- Use an alcohol swab to clean the area to be punctured. In most glucose meters, the fingertip will be pricked. However, with some gauges, you can also use your forearm, thigh, or fleshy part of your hand. Ask your doctor which area to use with your meter.
- Prick yourself with a sterile lancet to obtain a drop of blood. (If the tip of your finger is pricked, it may be easier and less painful to prick it on the side, not the fingertip.
- Place the drop of blood on the test strip.
- Follow the instructions to insert the test strip into your glucose meter.
- The meter will give you a number for your blood sugar level.
If you have a CGM, you will follow the insertion instructions that come with the monitor. Once warmed up, the transmitter sends the data wirelessly to your computer or smartphone.
What if I can't get a drop of blood from a finger stick?
If you want to get blood from the tip of your finger, try washing your hands in hot water to get the blood flowing. Then let your hand hang below the level of yourheartduring a minute. Prick your finger quickly and then bring your hand back below the level of your heart. You can also try slowly squeezing your finger from base to tip.
How often should I test my blood glucose?
Your GP will recommend how often to test. Test times are based on the type of medicine you take and how well your blood sugar levels are controlled. You may need to check your blood sugar more often at first. In turn, you will need to check it more often when you feel sick or stressed, when you change your medicine, or if you are pregnant.
What do I do with the results?
You need to keep track of your results. There are several ways to do it. You can write them down in a log book. You can use a small notebook or ask your doctor for a blood test log book. Depending on the type of monitor you have, you may be able to keep track of the results on your computer or smartphone. Whichever method you use, you may also want to keep track of what you've eaten , when you took medications or insulin, and how active you've been during the day. This will help you see how these things affect your blood sugar level. Talk to your doctor about what is a good range for your blood glucose and what to do if it is not in that range.
What time of day should I take the test?
Recommendations for the best time of day to test your blood glucose will depend on your medications, meal times, and blood sugar control. Your doctor can provide you with a chart that tells you when to check your blood sugar and how high it should be. Your doctor may also suggest different goals, depending on your situation.
What do my blood glucose levels indicate?
Schedule for the test It can be used to ...
Fasting blood glucose (FBG) overnight (3-4 am) Adjust medication or long-acting insulin
Before a meal Modify the food or medicine
1-2 hours after a meal Learn how food affects blood sugar levels (often the highest blood sugar levels of the day *)
At bedtime Adjust the diet or the medicine (last chance for the next 8 hours)
* Depends on the size of the meal and the amount of insulin in your medicine
Check your blood sugar level in the following cases:
- You have symptoms of low blood glucose (hypoglycemia). This includes dizziness, tremors, sweating, chills, and confusion.
- You have symptoms of high blood sugar (hyperglycemia), including drowsiness, blurred vision, frequent urination, and excessive thirst.
- You have a job where poor glycemic control could cause safety concerns.
- You need help deciding whether it is safe to drive or perform other tasks that require concentration if you are taking insulin or have had hypoglycemia in the past.
- You must learn how food, physical activity, and medicine affect your blood glucose level.
When should I check my blood glucose more often?
- If your diabetes medicine changes
- If you start taking other types of medicines
- If you change your diet
- If you change your exercise routine or activity level
- If your level of stress increases
- If you are sick When you are sick, even without eating, your blood sugar levels can be high, so testing is important.
Follow your doctor's testing recommendations during this time. Continue testing more frequently until you have maintained your blood glucose targets for at least 1 week. Or continue testing until your doctor tells you that you no longer need testing as often.
Tips on blood glucose tests
For BGM, you must:
- Pay attention to the expiration dates of the test strips.
- Use a large enough drop of blood.
- Check your meter batteries.
- Make sure your meter is configured correctly.
- Keep your meter clean.
For BGM and CGM:
- Follow the instructions for the test carefully.
- Write down the results and show them to your doctor.
Aspects to consider
Controlling your blood sugar level is critical to your overall health. Often the goal is to keep blood sugar levels low. But if they are too low, this can also put you in danger.
Hypoglycemia is the name of a condition in which the level of sugar in the blood is too low. Your blood sugar level can drop too low if you exercise more than usual or don't eat enough. You can also go too low if you don't eat on time or take too much insulin. Symptoms of hypoglycemia include:
- Fatigue
- Frequent yawning
- Difficulty speaking or thinking clearly
- Loss of muscle coordination
- Sweating
- Spasms
- Convulsions
- Sudden feeling of Fainting
- Pallor
- Loss of consciousness
How can I deal with an insulin reaction?
People with diabetes should carry at least 15 grams of a fast-acting carbohydrate with them at all times in the event of hypoglycemia or an insulin reaction. The following are examples of quick energy sources that can ease the symptoms of an insulin reaction:
- Regular soda (not diet): ½ to ¾ cup
- Fruit juice: ½ cup
- Dried fruit: 2 tablespoons raisins
- Milk: 1 cup
- Candy: 5 Lifesavers candies
- Glucose tablets: 3 tablets (5 grams each)
If you don't feel better 15 minutes after eating a fast-acting carbohydrate, or if your monitoring shows that your blood glucose is still too low, take another 15 grams of a fast-acting carbohydrate.
Teach your friends, co-workers, and family how to treat hypoglycemia, as you may need their help at times. Also, keep a supply of glucagon on hand. Glucagon comes in a kit with a powder and a liquid that you mix and then inject. Your blood glucose level will increase. If you are unconscious or unable to eat or drink, another person may give you ainjectionglucagon. Talk to your doctor about when and how to use glucagon.
If you use a CGM, remember that it collects data over many days. Even during the day, the data you see is from a few minutes earlier. Therefore, it is not the best option to show you what your blood sugar is at any given time. Sometimes you must use a fingerstick for an accurate and timely reading. These include when you are exercising and after you have taken insulin to correct a high glucose reading. Fingertips can also be a good backup for your CGM. Use them when your CGM sensor is warming up and when the sensor shows high or low readings. Also use them if you have symptoms of high or low blood glucose or if you suspect that your CGM is not working properly.
Questions to ask your doctor
- How often should I check my blood glucose level?
- What type of device should I use to monitor my blood glucose level?
- Should I take medicine to lower my blood sugar?
- Can you show me how to use a glucose meter?
- Should I keep track of my daily results?